Borderline Personality Disorder vs Bipolar: What's the Difference?
If you or someone you love has been told they might have borderline personality disorder or bipolar disorder, you’re not alone in feeling confused. These two conditions are among the most frequently misdiagnosed in psychiatry. At Zen Minds Psychiatry in Boston, we see patients who have lived for years with the wrong diagnosis, receiving treatments that simply didn’t fit. Getting the right answer changes everything.
This guide breaks down everything you need to know about borderline personality disorder vs bipolar disorder: what they are, how they differ, what causes them, and how they’re treated.
BPD vs Bipolar? An Overview
Borderline personality disorder (BPD) and bipolar disorder (BD) are both serious mental health conditions that involve intense emotional experiences. They are, however, fundamentally different in nature, timeline, and treatment.
BPD is a personality disorder — meaning it involves deep, persistent patterns in how a person perceives themselves, relates to others, and regulates emotions. Bipolar disorder is a mood disorder — defined by distinct episodes of mania (or hypomania) and depression that can last weeks to months.
What Is Borderline Personality Disorder (BPD)?
Borderline personality disorder is characterized by pervasive instability in emotions, relationships, self-image, and behavior. It typically begins in early adulthood and affects approximately 1.6% of the general population — though estimates in clinical settings run higher.
The ICD-10 code for borderline personality disorder is F60.3 (Emotionally Unstable Personality Disorder, borderline type). In the DSM-5, it is diagnosed when five or more of the following nine criteria are present:
- Frantic efforts to avoid real or imagined abandonment
- Unstable and intense interpersonal relationships (alternating between idealization and devaluation)
- Persistently unstable self-image or sense of self
- Impulsivity in at least two self-damaging areas (spending, sex, substances, reckless driving, bingeing)
- Recurrent suicidal behavior, gestures, threats, or self-harm
- Emotional instability due to a marked reactivity of mood
- Chronic feelings of emptiness
- Inappropriate, intense anger or difficulty controlling anger
- Transient, stress-related paranoid ideation or severe dissociation.
What Causes BPD?
The exact cause of borderline personality disorder is not fully understood, but research points to a combination of biological, psychological, and environmental factors:
- Genetics: BPD tends to run in families, suggesting a heritable vulnerability.
- Brain structure and function: Differences in areas of the brain that regulate emotion and impulse control have been identified in people with BPD.
- Trauma and early environment: A significant proportion of people with BPD report a history of childhood trauma, including emotional, physical, or sexual abuse, or prolonged neglect. An invalidating environment — one where a child’s emotional experiences are consistently dismissed — is a well-established risk factor.
- Emotional sensitivity: Many individuals with BPD appear to have a heightened neurobiological sensitivity to emotional stimuli from early in life.
BPD Symptoms in Teenage Girls
One of the most searched topics in this space is symptoms of BPD in teenage girls. BPD is rarely formally diagnosed before age 18 — clinicians are cautious because personality is still developing in adolescence — but early signs often appear in the teenage years and may look like:
- Intense and unstable friendships, often with dramatic falling outs
- Rapid and extreme emotional shifts tied to social situations
- Self-harm or threats of self-harm during emotional crises
- Feelings of emptiness or boredom that seem impossible to fill
- Impulsive risk-taking behavior (substance use, unsafe sex, reckless behavior)
- A poorly developed sense of self — not knowing who they are or what they want
If these patterns are present in a teenager you know, an evaluation with a qualified psychiatrist is essential. Early intervention with evidence-based therapy can significantly alter the long-term course.
What Is Bipolar Disorder?
Bipolar disorder is a mood disorder defined by episodes of mania or hypomania, typically alternating with episodes of depression. It is a biological illness with strong genetic ties. At Zen Minds Psychiatry, bipolar disorder treatment in Boston is one of our core areas of specialization. Dr. Chopra — dual board-certified in psychiatry and sleep medicine, and trained at Mayo Clinic — has over 20 years of experience managing Bipolar I, Bipolar II, and complex mood presentations.
There are two primary types:
- Bipolar I: Defined by at least one full manic episode lasting 7 or more days (or any duration if hospitalization is required). Depressive episodes are common but not required for diagnosis.
Bipolar II: Defined by at least one hypomanic episode and one major depressive episode. Full mania is absent. Bipolar II is frequently underdiagnosed and misidentified as recurrent depression.
Symptoms of Bipolar Depression
The depressive phase of bipolar disorder can look nearly identical to major depressive disorder, which is one reason accurate diagnosis requires a thorough psychiatric evaluation. Symptoms of bipolar depression include:
- Persistent sadness, hopelessness, or emptiness lasting two or more weeks
- Loss of interest in activities that previously brought pleasure
- Significant changes in sleep — often sleeping too much (hypersomnia), unlike the insomnia more common in MDD
- Low energy, physical heaviness, or slowed movement
- Difficulty thinking, concentrating, or making decisions
- Recurrent thoughts of death or suicidal ideation
Many patients presenting with depressive episodes benefit from a comprehensive evaluation. If you’ve tried antidepressants without success, it’s worth discussing whether a bipolar diagnosis could explain the picture.
Bipolar Disorder vs BPD: Side-by-Side Comparison
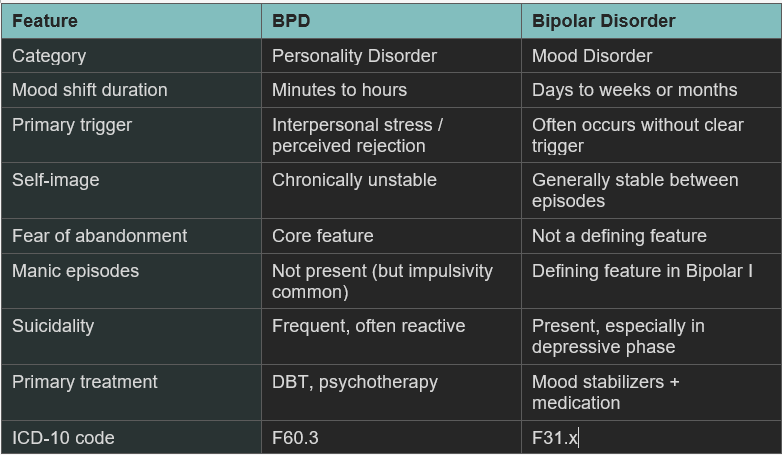
Can Someone Have Both BPD and Bipolar Disorder?
Yes. BPD and bipolar disorder can co-occur, and research suggests this comorbidity is more common than previously recognized — particularly between BPD and Bipolar II. When both are present, the clinical picture is more complex, and treatment must address both conditions simultaneously.
This is one reason why diagnostic precision matters so much. A psychiatrist who specializes in complex mood presentations and personality disorders is best positioned to disentangle the two and build an effective treatment plan.
Borderline Personality Disorder Test: How Is BPD Diagnosed?
There is no blood test or brain scan that diagnoses BPD. Diagnosis is clinical — meaning it depends entirely on a thorough psychiatric evaluation conducted by an experienced clinician. This typically involves:
- A structured clinical interview reviewing mood history, relationships, identity, and impulsive behaviors
- Validated screening tools such as the McLean Screening Instrument for BPD (MSI-BPD) or the Zanarini Rating Scale (ZAN-BPD)
- Review of prior psychiatric history and treatment responses
- In some cases, input from family members or close contacts
If you suspect you or a loved one may have BPD, don’t rely on online quizzes. A proper evaluation with a qualified psychiatrist is the only way to reach an accurate diagnosis — and to make sure the right treatment follows.
Borderline Personality Disorder Specialists in Boston
Finding a borderline personality disorder specialist in Boston who has experience with both BPD and bipolar disorder is critical. At Zen Minds Psychiatry, Dr. Amit Chopra offers comprehensive psychiatric evaluations designed to differentiate between these two conditions and co-occurring presentations. As an affiliated clinician at Massachusetts General Hospital and faculty member at Harvard Medical School, Dr. Chopra brings an exceptional depth of expertise to complex cases. Our psychiatric services page outlines the full range of conditions we treat.
Treatment: How Each Condition Is Managed
Treatment for BPD
Dialectical Behavior Therapy (DBT) is the gold-standard psychotherapy for BPD, developed specifically for this population by Dr. Marsha Linehan. It teaches four core skill sets: mindfulness, distress tolerance, emotion regulation, and interpersonal effectiveness.
Medication is not a first-line treatment for BPD, but it may be used to target specific symptoms such as emotional dysregulation, impulsivity, or co-occurring depression and anxiety.
Treatment for Bipolar Disorder
Bipolar disorder is primarily managed with mood-stabilizing medications — lithium, valproate, and lamotrigine are most commonly used. Atypical antipsychotics are also frequently part of the treatment plan. Therapy plays a crucial supporting role, particularly psychoeducation and CBT. At Zen Minds Psychiatry, our bipolar disorder treatment center in Boston integrates sleep medicine expertise into bipolar care — because circadian disruption and sleep abnormalities are both triggers and symptoms of mood episodes.
Frequently Asked Questions?
How do I know if I have BPD or bipolar disorder?
You can’t reliably distinguish the two without a proper clinical evaluation. Both involve emotional intensity and impulsivity, but they differ in the duration and nature of mood shifts, and in what triggers them. A psychiatrist with expertise in personality disorders and mood disorders is the right person to make this determination.
Is BPD worse than bipolar?
Neither condition is “worse” than the other — both can be seriously impairing without proper treatment. BPD tends to affect interpersonal functioning and identity more pervasively, while bipolar disorder involves more discrete episodic swings. Both are highly treatable with the right approach.
Can BPD go away on its own?
Research suggests that BPD symptoms do remit over time for many people, particularly with effective treatment. DBT and related psychotherapies significantly accelerate this process. Bipolar disorder, in contrast, is typically a lifelong condition that requires ongoing management.
What is the ICD-10 code for borderline personality disorder?
The ICD-10 code for borderline personality disorder is F60.3, classified under Emotionally Unstable Personality Disorder. In ICD-11, it is reclassified under Personality Disorder with a prominent pattern specifier.
Can antidepressants make BPD worse?
In some cases, yes. Antidepressants prescribed without a correct diagnosis can worsen emotional instability in BPD, and in undiagnosed bipolar disorder, they can trigger manic or mixed episodes. This is one of the key reasons accurate diagnosis must come before medication decisions.
When to Seek Help in Boston
If you are struggling with intense emotional swings, unstable relationships, or feel like no treatment has worked — an accurate diagnosis from an experienced specialist is the most important first step. Book a consultation at Zen Minds Psychiatry in Boston to discuss your symptoms with Dr. Chopra. We offer both in-person and telepsychiatry visits across Massachusetts.
Zen Minds Psychiatry serves patients across Boston and Massachusetts with in-person and virtual psychiatric care. Dr. Amit Chopra, MD — Harvard Medical School faculty, MGH-affiliated, Mayo Clinic-trained — specializes in complex mood and personality disorder presentations. Call us at (626) 594-6042 or book online.



